Gut Health and Brain Health: Understanding the Gut–Brain Connection
Apr 07, 2026How the Gut-Brain Axis Dictates Your Mood and Mental Clarity
The health of your digestive system influences mood, energy, and mental clarity through the gut-brain axis, a bidirectional communication highway linked by the vagus nerve and biochemical signaling. Root causes of brain fog and low energy often reside in gut microbiome imbalances and systemic inflammation, which disrupt the production of key neurotransmitters like serotonin. Clinically, addressing these digestive triggers is essential because an imbalanced gut can perpetuate a cycle of chronic stress and cognitive dysfunction.
While many view digestion and cognition as separate functions, they are biologically inseparable. Contributing factors such as metabolic dysfunction, hormonal shifts, and chronic inflammatory responses often manifest as "mental" symptoms, yet they originate in the gut lining and microbiome. When the delicate ecosystem of your gut is compromised by poor diet or lifestyle stressors, it directly impairs the chemical messengers required for focus and emotional stability.
As an IFMCP-certified practitioner, Dr. Jennifer Engels specializes in identifying these hidden connections. At WeCare Frisco, we move beyond surface-level symptom management by utilizing advanced functional testing to assess microbiome diversity, food sensitivities, and intestinal permeability. Our personalized care plans focus on targeted nutritional interventions and vagus nerve support, helping you break the cycle of gut-driven fatigue and reclaim your mental edge. Visit our Foundational Assessment page to learn more.
It may sound surprising, but what happens in your digestive system can significantly influence how you think, feel, and function each day. Most people assume the gut and brain operate independently, one handling digestion, the other handling thought. In reality, they are in near-constant communication, and the health of one directly shapes the health of the other.
This relationship is known as the gut–brain connection, and understanding it can help explain why digestive issues so often create symptoms that seem entirely unrelated to the stomach.
A Two-Way Communication Pathway
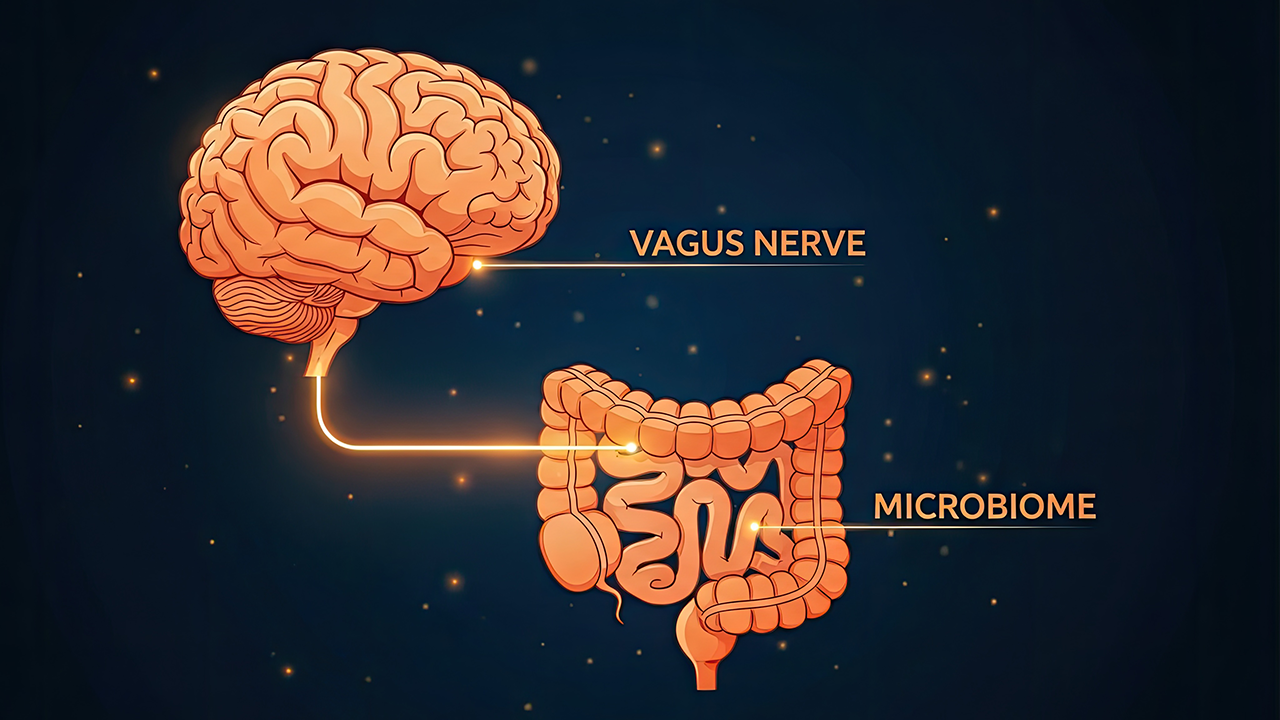
The gut and brain are linked through what scientists call the gut–brain axis. At the center of this network is the vagus nerve, a long, branching nerve that runs from the brainstem down through the chest and into the abdomen. It acts as a major communication highway, carrying electrical signals and chemical messengers in both directions between the brain and the digestive tract.
From the top down, the brain regulates digestion, appetite, and the movement of food through the gastrointestinal tract. From the bottom up, the gut sends signals back to the brain about inflammation, nutrient levels, and the condition of its internal environment. Because this communication is constant, disturbances in the digestive system can ripple upward, influencing mood, focus, and mental clarity, often in ways that are difficult to trace back to their source.
The Role of the Gut Microbiome
Alongside the vagus nerve, another major player in the gut–brain connection is the gut microbiome: the vast ecosystem of trillions of bacteria and microorganisms that live in the digestive tract. Far from being harmful, many of these organisms are essential to good health. They assist with digestion, help produce key vitamins, and play an active role in regulating the immune system.
Perhaps most remarkably, gut bacteria also influence the production of brain chemicals that regulate mood and cognition. Roughly 90–95% of the body’s serotonin - a neurotransmitter widely associated with emotional well-being - is actually produced in the gut, not the brain. When the microbiome becomes imbalanced, this chemical production can be disrupted, potentially contributing to symptoms like low mood, fatigue, and difficulty concentrating.
A healthy, diverse microbiome supports both digestive health and stable brain function. An imbalanced one can quietly undermine both.
When the Gut and Brain Fall Out of Balance
Because the gut and brain are so tightly linked, symptoms often appear in both places at once. Individuals experiencing bloating, irregular bowel habits, or chronic gut inflammation frequently also notice fatigue, brain fog, or increased stress responses and may not connect these to their digestive health.
The relationship also runs in the opposite direction. Stress is well known to affect digestion: the “butterflies in the stomach” many people feel before a nerve-wracking event is a familiar example of the brain influencing the gut. When stress becomes chronic rather than occasional, it can interfere with normal digestive processes, alter the microbiome, and contribute to ongoing gut symptoms. Over time, this situation can create a cycle in which gut disturbance and mental stress reinforce one another.
Practical Steps to Support a Healthy Gut–Brain Connection
There are several evidence-informed ways to begin supporting both digestive and brain health:
- Eat a diverse, nutrient-dense diet rich in fiber, vegetables, and fermented foods such as yogurt, kefir, kimchi, or sauerkraut, which support a healthy and varied microbiome
- Manage stress consistently — not just acutely. Practices like diaphragmatic breathing, meditation, or even regular walking can support vagal tone and reduce the chronic stress load on the gut
- Prioritize sleep, as gut bacteria follow circadian rhythms and poor sleep is associated with microbiome disruption
- Limit unnecessary use of antibiotics and highly processed foods, which can reduce microbial diversity
- Get a personalized evaluation since the most effective approach is one tailored to your individual health history
A Functional Medicine Approach
At WeCare Frisco, we take a Functional Medicine approach to digestive health. Rather than addressing symptoms in isolation, Functional Medicine looks deeper to identify the root causes affecting the gut–brain connection. For many patients, this means a meaningful shift: instead of managing discomfort, they begin to understand and resolve it.
The underlying factors often include:
- Diet and nutritional balance
- Inflammation within the body
- The health and diversity of the gut microbiome
- Stress levels and lifestyle habits
- Possible food sensitivities or intolerances
By addressing these root causes, many patients experience improvement not only in digestive symptoms but also in overall energy, mood, and mental clarity.
When to Seek Guidance
If you are experiencing ongoing digestive discomfort, fatigue, brain fog, or other symptoms negatively affecting your life, it may be time to look more closely at the health of your gut–brain axis. While common, these symptoms are not something you simply have to live with.
Through a Foundational Assessment at WeCare Frisco, we can take a thorough look at your health history, discuss your current symptoms, and develop a personalized plan to help you restore balance. The assessment is the starting point for understanding what is driving your symptoms and what it will take to resolve them.
Click here to schedule your Foundational Assessment at WeCare Frisco. We’re here to help you take the next step toward improving the quality of your life through better digestive health.



